
Soy as Part of Your Breast Cancer Treatments
Few things seem as controversial as the intake of soy. This has always seemed strange to me given that the bulk of the research on soy that I have come across is overwhelming positive. And yet, if you ran an Internet search for soy, the first page is likely to come back with results about how soy will give boys breasts and pretty much ensure that a woman will develop breast cancer.
This last one, we will see in a moment, is a bit surprising given the research I will share with you.
What I believe happens is that few people truly dig out the research that others mistakenly quote and this bad information just gets passed on. I remember an article several years back that was damning towards soy. When I checked the 11 or so references in the article, only ONE was not favorable to soy (and this one was on defatted soybeans in rats, just in case you were looking to run out and buy defatted soybeans….). The rest of the articles were in favor of soy and good health.
One of the articles that has gained almost biblical status in the anti-soy groups looked at soy use in teenage boys. The combined results of the study showed that soy increased estrogen levels. BUT, what happened in this study was that one single teenage boy had an unusual response to soy and his estrogen levels jumped. The other teenage boys? They showed an increase in testosterone-completely contrary to how most reference this study.
There are a few important things that I do need to point out.
First, when I talk about soy, I always mean NON-GMO, unprocessed soy. This means organic or certified GMO free and no soy by-products like TVP (textured vegetable protein) and no soy burgers or soy dogs.
Next, there are some studies that found that using soy-based infant formulas did raise estrogen levels in infants. This should be irrelevant because breast feeding is always, always going to be the best option. Anything less is, of course, going to be problematic. While one may choose to throw virtual stones at infant soy formula, there are equally as many problems with cow’s milk based formulas.
There are many ways that soy protects against being diagnosed with breast cancer, but the more powerful compounds in soy are the isoflavones. I won’t go into how the gut bacteria and antibiotics affect how well your body will use these compounds, but you can refresh your memory by reading back through the section on soy in the first part of this Breast Cancer Myths article by clicking here.
Lastly, we need a clarification on exactly how soy works in the human body. At some point, the compounds in soy were labeled “phytoestrogens.” This is incorrect. A better term would be “plant derived hormonal modulators.”
Yes—the compounds in soy do attach to estrogen receptors, but when they do, they have 1/1000th the effect that estrogen does. This means that, when lots of estrogen is present (which would lead to higher risk of breast cancer) and soy compounds hog up the landing space on this receptor, there is 1/1000th the message sent into the cell nucleus to divide.
If, on the other hand, there is almost no estrogen present (such as after menopause or in an infant) this is still some type of stimulation on the receptor—more than nothing.
This being said, let’s look at how soy does or does not affect the risk of developing breast cancer and chance of survival if you are diagnosed with breast cancer.
Soy and Breast Cancer Risk
There has been a long-held belief that Asian women have a much lower risk of being diagnosed with breast cancer and that their increased intake of soy was at the heart of this dietary protection. There have been quite a few studies over the years that have confirmed that soy does indeed protect against being diagnosed with breast cancer (keeping in mind the factors we have already covered).
What is interesting is that an increased intake of soy as an adolescent, which is a very important period for the development of breast tissue, can lower a woman’s lifetime risk of breast cancer.
One study looking at a group of almost 600 women diagnosed with breast cancer and a similar group of women who did not have breast cancer to see if soy intake made a difference.
In women who had the highest childhood intake of soy, there was an astounding 60% lower risk of being diagnosed with breast cancer. Sixty percent! Actions as a child had the ability to lower the risk of breast cancer over a lifetime.
The protection for those women who had higher intakes as an adolescent were less striking but still impressive: 20% lower risk of being diagnosed with breast cancer.
The study also looked at the adult intake of soy to see if this had a protective effect as well and found that, in women with the highest intakes of soy, there was a 24% lower risk of being diagnosed with breast cancer. While not as protective as childhood soy intake, it’s still pretty darn impressive for one single dietary choice.
Another study also looking at almost over 73,000 women in China to see if soy intake during different phases of life affected the risk of being diagnosed with breast cancer.
Much like the prior study, higher intakes of soy during adolescence led to a 43% lower risk of being diagnosed with breast cancer.
In this study, however, researchers found that that the protection from higher soy intakes as an adult was stronger than having more soy as an adolescent. There was a 59% lower risk of being diagnosed with breast cancer in women who had the highest intakes of soy as an adult.
Not surprisingly, women who consumed a high amount of soy foods consistently during adolescence and adulthood got the greatest protection from premenopausal breast cancer. None of the protections from soy intake were present for a postmenopausal diagnosis of breast cancer.
The take home message here is that lifelong intakes of soy (again—non-processed, non-GMO) have been shown to be strongly protective against being diagnosed with breast cancer. If you remember when we talked about the enterolactones that are made from the compounds in soy by the bacteria in the gut. It takes time for these bacteria to grow and gain a foothold. This is likely why long term intake of soy is so protective—it gives time for the right bacteria to grow and thrive in your gut to make the most powerful anti-breast cancer compounds available.
But if soy can help prevent breast cancer, can it also help improve outcomes and survival if you are diagnosed with breast cancer?
Soy and Breast Cancer Survival and Breast Cancer Recurrence
For as long as I have been in practice, oncologists have been telling their breast cancer patients to avoid soy in the mistaken belief that it can worsen cancer outcomes. As I will show you in this section, this advice flies in the face of research that shows just the opposite.
In the last section, the research from the Shanghai Breast Cancer study showed that soy played a role in lowering your risk of being diagnosed with breast cancer. This same study group was evaluated to see if soy intake played a role in outcomes in just over 5,000 women who had been diagnosed with breast cancer and underwent some type of surgery to remove the lesion.
One of the main concerns that this study addressed was whether the isoflavones in soy had an interaction with Tamoxifen that may have derail Tamoxifen’s “protective” effect on breast cancer recurrence (I have covered this fallacy in last week’s part of this article).
Here’s what the details:
- All women were surgically treated.
- In women with the highest intake of soy protein there was a 29% lower risk of dying and a 32% lower risk of breast cancer recurrence.
- This protection was present regardless of whether the breast cancer was estrogen receptor–positive or –negative.
- This protection was also present in both users and nonusers of tamoxifen.
Keep in mind that this protection is from something as simple as a dietary choice. There is NO toxicity. Some chemotherapeutic treatments don’t even promise a benefit on survival (disturbingly truthful) but have very significant toxicity.
In case this isn’t enough to sway your oncologist to let you eat soy (as if he or she were monitoring your every meal…), another study adds further weight to the evidence. Researchers found, that, in over 5,000 women diagnosed with invasive breast cancer (again—the worst kind of breast cancer with worse outcomes) those who took in more than 10 mg of isoflavones from soy per day had a:
- 13% lower risk of dying overall
- 17% lower risk of dying from breast cancer
- 25% lower risk of breast cancer recurrence
To get 10 mg of isoflavones in soy per day, this is the equivalent of 1.5 cups of soy milk, 1.5 ounces of tofu (pretty much a cube) or like 1/8 cup of edamame. Isoflavones are also found in other foods in the same family, but soy contains the highest levels. Overall, though, these serving sizes are pretty easy to add to your daily diet.
The Women’s Healthy Eating and Living (WHEL) Study was a large experiment looking at how much lifestyle changes in over 3,000 diagnosed with invasive breast cancer could make a difference in breast cancer recurrence and death.
The results of this study were very consistent with the results of the Shanghai study noted above:
- Women at the highest levels of isoflavone intake (more than 16.3 mg per day, or the amount found in at least one-half cup soymilk or 2-oz tofu) had a 54% lower risk of death.
- Women using tamoxifen had the same protection, and the results even suggested that women who had ever used tamoxifen might have had even stronger protection from soy intake.
- The protection from soy did not differ based on hormone receptor status of the tumor.
Hopefully you are beginning to see that, if your oncologist told you to avoid soy during your cancer treatment, it’s likely that he or she has not cracked a medical journal RELATED TO HIS OR HER FIELD in quite a few years. Not good given that it is your life at stake.
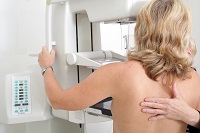
Mammography Myths
I thought I’d save the best portion for last. This will be, unquestionably, the most controversial aspect of this entire 15,000+ word article.
It is also going to be the aspect of the breast cancer culture that you have not heard the balanced story on. I’ve hinted at little tidbits so far, but I’ll bring it all together.
And there is one thing that you need to understand VERY clearly. Breast cancer is a massively big business. From mammography centers to surgeons to drug companies who sell expensive chemotherapeutic drugs to radiation oncology centers.
And this is all fed by an engine that promotes screening. How much money have the major breast cancer support and awareness groups raised to promote the culture of breast cancer screening?
This next section will cover some very specific factors as they relate to mammography breast cancer screening:
- Just how effective is mammography at lowering the risk of invasive breast cancers and breast cancer deaths?
- What are the harms of routine screening mammography?
This last section may blow apart what you’ve been led to believe as it relates to our entire culture on breast cancer awareness and screening mammography.
Mammography = No Change in Deaths
The “cancer culture” chooses early cancer detection instead of prevention and calls it a cure. I can sum it up no more clearly than that. When medicine talks about breast cancer “prevention” the answer that comes to the top is mammography. But mammography is, in no way, shape or form, “prevention.” It is early detection of a problem already present.
In the first part of this article, I’ve covered just how much we know about how to prevent breast cancer. Hopefully you realize just how powerful lifestyle is at lowering your risk of being diagnosed with breast cancer in the first place.
The big argument about “screening” using mammography and early detection and aggressive treatment of any lesions that are found is that it saves lives.
Breast cancer screening saves lives.
Not much to debate there? You might be surprised.
One study looked at the different rates of mammography across the US to see if this had an impact on breast cancer survival rates. In a very large study of 16 million women 40 years of age and older.
In other words, if mammography is slashing breast cancer mortality rates and saving lives, then the areas of the country that have higher rates of mammography screening should have lower breast cancer deaths. Here’s what they found:
- As expected, the areas of the country that had higher rates of screening had higher rates of breast cancer.
- However, screening rates had no impact on breast cancer mortality rates.
- For every 10% increase in screening rates there were 16% more breast cancer diagnoses but no equivalent drop in breast cancer deaths.
- More screening led to higher rates of small breast cancers (≤2 cm) but there was no corresponding decrease in large breast cancers (>2 cm) found (in other words–more screening didn’t lead to cancers being detected earlier instead of advancing and being found at a later stage).
To put it more plainly, this large study found evidence that mammography does NOT save lives, but does lead to the over-diagnosis of small breast lesions.
Another study done on almost 90,000 women in Canada aged 40-59 were randomly put into either an annual mammography group or no mammography group. Women in the mammography group that were ages 40-49 also had annual breast exams, while those in the control group only had a single exam followed by whatever normal care they would receive. All women who were ages 50-59 in both groups received annual physical breast examinations.
This group of women were then followed for the extended period of 25 years to see how many died from breast cancer. Here’s what they found:
- In the first 5 years of the study, 666 invasive breast cancers were diagnosed in the mammography group and 524 in the controls. Makes sense—with more screening you will find more cancers.
- In this same time period, 180 women in the mammography group and 171 women in the control group died of breast cancer. In other words, the risk of dying of breast cancer was almost identical.
- After the full 25 years, 3250 women in the mammography group and 3133 in the control group were diagnosed with breast cancer and 500 in the mammography group and 505 controls died of breast cancer.
There was no difference in those who received a mammography versus those who did not.
The conclusion of the authors says it all: “Our data show that annual mammography does not result in a reduction in breast cancer specific mortality for women aged 40-59 beyond that of physical examination alone or usual care in the community. The data suggest that the value of mammography screening should be reassessed.”
OK.
So, mammography didn’t make a shred of difference in breast cancer outcomes. So why not let everyone make their money and keep everything running as it is. Everyone’s happy.
Right?
Breast Cancer “Overdiagnosis” – Waking Up to the Reality
Cancer screening is arguably one of the more hotly debated procedures in medicine today. However, when we get emotional about cancer screening is when we lose touch with the benefit vs harm balance.
It all seemed to start with the USPSTF guidelines in 2009 to not screen women in their 40s for breast cancer using mammography. There was an uproar from the American Cancer Society, various radiological societies and women everywhere. Early detection is key to breast cancer treatment and has been drilled into our heads to the point that few women would even consider waiting until they are 50 for their first mammogram.
But to make a fully informed decision, we need to understand all the facts. Does early detection of a future invasive breast cancer save lives?
Yes.
But is this balanced out by the harms that mammography causes?
First, there are a few important things to consider:
- A large percentage (57%) of breast lumps are identified by self exam or by accident and NOT by mammography.
- The rate of false negatives is also high, leading to lowered quality of life and extreme stress levels (more on this in a bit).
- A large chunk of breast lesions found on mammography may resolve on their own. In other words, we are treating a lesion that will go away on its own and treatment had nothing to do with the outcome. Yet mammography gets credited with a life saved.
- When mammography is done, the risk of invasive surgery such as a mastectomy goes up. In Norway, this number went up a whopping 70%, but there was no improvement in breast cancer outcomes.
Most people do not even understand that there is a downside to mammography. But, statistically this is not true. Your risk of being harmed by a mammography, most notably in those younger than 50, is much greater than the risk of your life being saved.
The first study to really dig into this aspect of mammography came out from Norway. Researchers were able to tease apart the data from before mammography was implemented and compare it to data from after mammography was implemented on a broad scale.
The estimates were that mammography led to overdiagnosis in 15-25% of women in whom cancer was found on testing. These are women who would have had procedures done that did not need to be done. The costs and harms associated with this are staggering.
These costs and harms are not just about the dollars that we spend on the testing itself. The non-financial costs are far greater than anything you could possibly calculate on your smartphone. To give you an idea of just home massive these costs are, one study evaluated the harms that mammography screening creates by diagnosing lesions that were NEVER GOING TO BECOME CANCEROUS. Here are a few of the findings:
- The introduction of screening mammography in the US doubled the number of cases of early-stage breast cancer that are detected each year.
- Despite this massive increase in discovered breast cancer, the rate at which women are diagnosed with late-stage cancer has decreased by only 8%.
- Overall, for every 100,000 women, mammography led to 122 women being diagnosed with early stage breast cancer, but only 8 of these would have progressed to advanced cancer.
With some number crunching, the authors estimated that, in the past 30 years, 1.3 MILLION women were diagnosed with breast cancer that would not have progressed. In 2008 only, this number was 70,000 women (31% of all breast cancers diagnosed).
And we all know what happens to any women who is diagnosed with breast cancer: additional testing, biopsies and potential subsequent treatment with surgery, radiation, chemo or some combination thereof.
1.3 million.
Of course, one side of the argument would be that we just don’t know which 8 of these 100,000 women are going to progress to advanced cancers. This is certainly valid. But how much more money would we be able to throw at research to answer this question if we weren’t wasting billions more on treatments that aren’t needed?
In the 2nd part of this article, I covered the different types of breast cancers as well as breast lesions like DCIS. I’ve covered the fact that DCIS is not cancer, but is a risk factor for future invasive cancer.
Despite the fact that DCIS is not cancer, we treat it like it is. The approach has been compared to the military’s approach of “shock and awe” using surgery, chemo, radiation and long term drug therapy like tamoxifen.
Let’s put this in perspective.
- You have an abnormal PAP screen. Your doctor immediately gets you in for a surgical removal of your uterus and ovaries, followed by chemo and radiation.
- Your dermatologist removes a small lesion on your skin by burning it off, just to be safe. But, just to be REAL safe, you undergo PET scans and biopsies to make sure nothing has spread followed by chemo and radiation.
- You come out of your colonoscopy and your GI doc said they took out a small polyp. He then immediately schedules you for a colon resection with follow up chemo and radiation.
Of course these 3 scenarios sound like massive overkill a ridiculous approach to treatment. But they are NO different then what we do with ductal carcinoma in situ. When women are told that they have cancer the entire psychological impact of the “C” word comes into play.
Every statistic related to DCIS will tell you that it accounts for about 20% of breast cancer cases and that the incidence of DCIS has been increasing over the past few decades, which just so happens to mirror the public health recommendations for mammography.
As I have mentioned, despite more women being diagnosed with DCIS and more women getting breast cancer treatments, the deaths from breast cancer have not changed.
Just in case you think that taking an aggressive stance on treating every breast lesion we find, this review of routine mammography in over 700,000 women aged 40-59 may help put everything into perspective. Here’s what they found:
- 11% of the screening mammograms were false positives.
- This translates to 3.2 million women receiving false positive mammograms each year across the US, at a cost of $2.8 billion annually (yes—with a “B”).
- Of the true cancers detected, with an accepted overdiagnosis rate of 22% (based on previous studies),20,116 women would be overdiagnosed with invasive breast cancer, at a cost of $1 billion each year.
- For DCIS, the rate of overdiagnosis is a shocking 86%.With these numbers for DCIS the estimated the cost of DCIS overdiagnosis nationwide to be $243 million.
FOUR BILLION ANNUALLY. These are serious numbers. This may help you understand why so many groups were against the recommendations to stop routine screening women under age 50. There’s a LOT of money to be lost. These groups continue to shout from the mountaintops that routine screening should be done and the mounting evidence demonstrating significant harm from routine mammography is all hogwash.
No one seems to be taking you, the female patient, into consideration.
The best discussion between you and your doctor would be one that discusses the very real and very likely chance that you will be diagnosed with a condition that will never harm you. This should take into account your family history, lifestyle factors and age. This discussion should then naturally steer towards what lifestyle choices you should choose to dramatically lower your personal risk of breast cancer.
If this is NOT the discussion you are having with your primary care physician, then maybe it’s time to find a new one.
Despite All of This, Emotion Rules on Breast Cancer Treatments
There is no doubt that there is a high degree of false positives with mammography. The psychological damage (which leads to a lowered perceived quality of life), additional cost and additional harms associated with radiation exposure and biopsy procedures (such as fine needle aspirations) are not to be ignored.
Mammography itself is a risk factor for cancer because of the radiation exposure.
Somewhere just above or below 50% of breast cancers are NOT detected initially via mammography, but rather through accident or deliberate self-examination.
Furthermore, although the number is always up for debate, at least 22% of the lesions found on mammography would be taken care of by the immune system. Imagine the numbers of women exposed to surgery, chemotherapy and radiation for a cancer that would never have grown. THIS is the true problem with mammography being recommended too early.
Despite all of this, when women aged 39-49 were asked to evaluate their own personal risk for getting breast cancer and their desire to get a mammogram before aged 50, the results were totally out of line with what reality is.
- 88% of the women overestimated their risk of breast cancer
- 89% want to be screened before age 50
Despite everything we know about breast cancer and breast cancer screening, women throw rational thought out the window and opt for the emotional approach (at least in this study…).
At to this over-reliance on mainstream medicine is the concept that the general public does not even realize you can prevent breast cancer. This is all despite millions upon millions of dollars raised in the name of breast cancer awareness.
Conclusion
Hopefully this rather long, drawn out article has at least opened your eyes to the reality of breast cancer awareness, prevention and treatments (or rather—need for treatments).
When we are talking about cancer it is never an easy decision. Your life or the life of someone you love may hang in the balance.
Or, it may not hang in the balance, but you’re led to believe that it does.
Overall, there are a few clear take home messages:
- Breast cancer is hugely, positively preventable in almost all cases.
- Breast cancer screening with mammography does not save lives above other methods of screening like breast self-exam and clinical breast exams.
- There are extreme downsides to relying on screening as your only method of “preventing” breast cancer. In other words, what you DO know may hurt you.
For me, the answer is ALWAYS lifestyle. There is, and will never be, a better answer when it comes to breast cancer prevention and breast cancer treatments. If you didn’t make the changes before you were diagnosed, you better damn well make them after. It’s never too late, and without changing the lifestyle that put the cancer there in the first place, it will only be a matter of time before your time runs out.
That may sound harsh, but if your life is not worth making some simple lifestyle changes and sticking with them beyond January 20th of the new year, there will be a price to be paid. If you’ve survived breast cancer, you’ve been given a second chance.
Not a second chance to live in constant fear of recurrence, but a second chance to revamp your lifestyle and fight off cancer from within.
Feel free to share your experiences, hopes and survival stories in the comments below. And thanks for sticking around til the end.
 Sign up for Bogash Life ‘N Balance and instantly receive a free copy of the eBook:
Sign up for Bogash Life ‘N Balance and instantly receive a free copy of the eBook:
Dr. Bogash, thanks so much for taking the time and energy to devour and assimilate the research and to write this comprehensive summary. I will share it with my family and my patients.
I wish you had discussed mammography for women over 59. Doesn’t anyone study us?
I found my own lump in 1989, when I was 44. It did not show up on a mammogram a year earlier. Although it was hormone receptor positive for both estrogen and progesterone, and was stage 1, I was given a lumpectomy, chemo and radiation. The chemo included Adriamycin which has life long negative consequences. I totally changed my diet afterwards. For a while I ate soy products, which apparently caused me to get IBS. Eliminating them helped resolve it, and eliminating gluten too cured it. Food is powerful and one size does not fit all. I eat strictly organic now too. I have also used bioidentical progesterone cream, per Dr. Lee, for 20 years. I have had no recurrences. I am debating whether to get any more mammograms.
It’s always awesome to hear when people understand and adopt lifestyle changes to help deal with chronic diseases like cancer. It is the ONLY way to truly address the condition in the long run. As far as studies in your age group…..you are absolutely correct. A big problem is that false positives go up with age, and the article goes into just how dangerous THAT can be. https://www.ncbi.nlm.nih.gov/pubmed/24691609
Dr. Bogash